Super-Heavy Periods? This Could Be Why…
 Illustrated By Ly Ngo
Illustrated By Ly NgoBy Kendall McKenzie
What Is PCOS?
Polycystic Ovary Syndrome — aka PCOS — is a hormonal disorder. People with PCOS don’t ovulate every month, and their ovaries produce more androgens (“male” hormones) than normal.
 Illustrated By Ly Ngo
Illustrated By Ly NgoWhat Are The Signs Of PCOS?
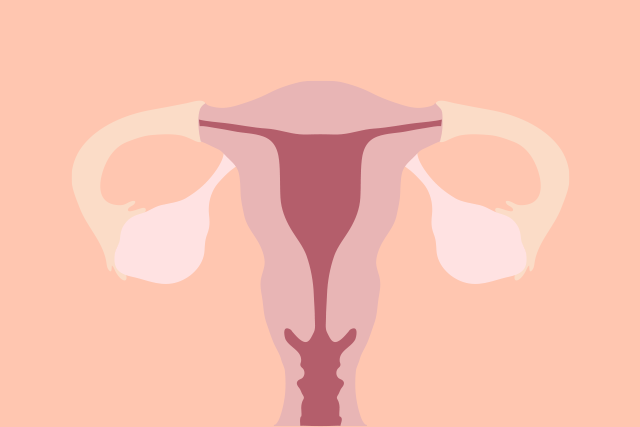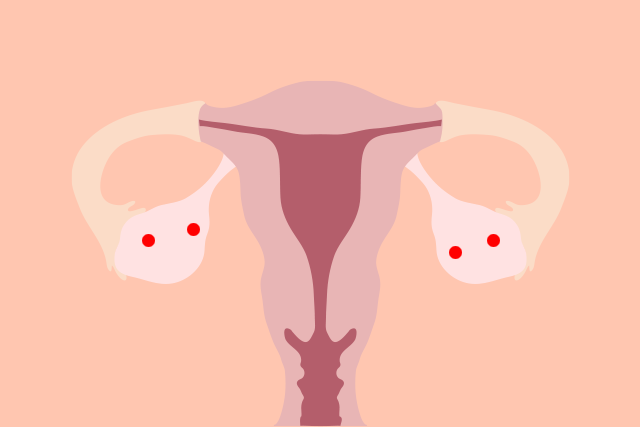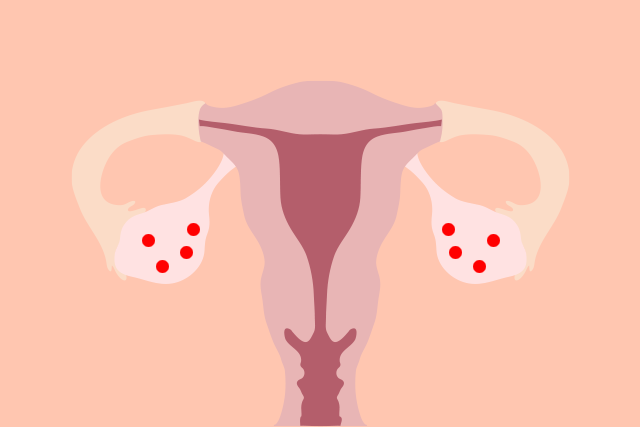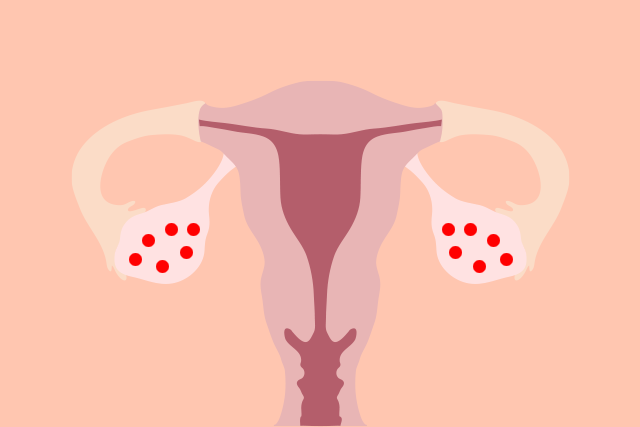
PCOS gets its name from the many small ovarian cysts commonly seen on ultrasounds in people with the condition (polycystic = lots of cysts). Normal-functioning ovaries contain immature eggs that get released into the fallopian tubes once they’re fully developed (hello, ovulation!). But, PCOS changes the balance of hormones necessary for ovulation, and the immature eggs are left behind as cysts on the ovaries. Other signs and symptoms of Polycystic Ovary Syndrome include:
AdvertisementADVERTISEMENT
-Irregular and/or infrequent periods
-Increased body and/or facial hair (called hirsutism)
-Skin issues: acne, oil, dandruff, skin tags
-Thick or dark skin patches on the neck, arms, back, breasts, or thighs
-Unexplained weight gain and/or trouble losing weight, especially around the waist
-Balding or thinning hair
-Infertility
There is no single test for PCOS; diagnoses are usually made based on the symptoms you’re experiencing, blood tests, and an exam. PCOS can go undetected for a long time because the signs vary from person to person.
 Illustrated By Ly Ngo
Illustrated By Ly NgoWhat Causes PCOS?
We don’t know what, exactly, causes PCOS. But, it’s believed that hormonal imbalance messes with the normal function of the ovaries, leading to PCOS symptoms. It’s often associated with insulin resistance, which is why diabetes and other metabolic disorders go hand-in-hand with PCOS — excess insulin is believed to increase androgen levels. And, sometimes ovaries just naturally produce more androgens, causing PCOS symptoms. Genetics may also be a factor.
 Illustrated By Ly Ngo
Illustrated By Ly NgoHow Does PCOS Impact Your Health?
Having PCOS increases your risk for diabetes and cardiovascular issues such as high blood pressure and high cholesterol. PCOS may also cause irregular periods, which increases the risk of endometrial (lining of the uterus) cancer.
Pregnant women with PCOS have higher rates of miscarriage, gestational diabetes, preeclampsia (high blood pressure), and premature delivery. Their babies have increased chances of dying during or right after birth, or spending time in intensive care.
The health problems that PCOS can lead to are definitely serious, but you can reduce your chances of developing them by following your nurse/doctor’s recommendations. And, the earlier you’re diagnosed with PCOS, the better; treating it ASAP helps prevent problems in the future.
AdvertisementADVERTISEMENT
 Illustrated By Ly Ngo
Illustrated By Ly NgoHow Do I Treat PCOS?
There’s no cure for PCOS, but it can be managed by a variety of treatments. Because people’s symptoms, health risks, and needs (such as whether you’re trying to prevent pregnancy or get pregnant) vary, so will treatment plans. Sometimes, simply eating healthy, exercising, and/or losing weight can help lower blood sugar, which normalizes the hormone balance to some extent.
PCOS is often treated with birth control pills, because they contain hormones that address some of the most common symptoms. For example, progestin-only methods can regulate your period and reduce the risk of endometrial cancer. Methods that contain both progestin and estrogen do the same, and can also help with acne and hair growth. Anti-androgen pills are sometimes prescribed to ease the effects of excess testosterone, and diabetes medications may help lower testosterone production. For people with PCOS trying to become pregnant, fertility treatments can stimulate ovulation.
Most symptoms can be reversed, or at least kept in check, with proper treatments and self-care. If you think you may have PCOS, get checked out by a nurse or doctor so they can tell you the best way to manage the effects and prevent serious health problems down the line.
AdvertisementADVERTISEMENT






